By Carol Masshardt
There are many options for talented nurse practitioners in a field with great need and short supply, and South Boston Community Health Center’s Jocelyn Guggenheim, RN, MS, CPNP, could be a leader in any of them.
“I started eleven years ago as a NP student and refused to leave,” she joked, adding “it is really close to the truth, and I didn’t even know then how much my role would change.” Clearly focused, practical, and analytic, a rare combination of skills, it is no mystery why she also was appointed as Chief Operating Officer in October 2021.
A Brandeis University graduate with an English degree, she went on to Northeastern University for a challenging combined RN/NP program, and worked in a variety of intensive, hospital-based positions in pediatric nursing. She honors each opportunity she has had, but the health center became the compelling core of her work, and where she devotes her heart and mind each day.
“It is a special place, and I knew it when I walked in. I met with Alison Marshall those many years ago, and it was the way she talked about it that was different. It’s fantastic work, and then and now, it attracts people with special energy,” she said. The community, the nature of relationships with patients and providers and the team kept her there and she grew and learned from patients in a dynamic environment, and then COVID-19 struck.
“I’m not sure there was anything that didn’t change,” she said in a unique way of mentally scanning and examining many details of multiple systems. “It forced us to re-think everything, waiting rooms, PPE, questions we asked, treatment provided, staffing, who could be on site and how to evaluate our own health and safety for others. Coming to work with minor symptoms was something we may not have thought much about before, but the whole barometer changed,” she said.
Known and comfortable practices transformed to new and untested ways of how to best operate. “We cancelled all appointments one day, and tried to re-configure physical space and the processes,” she explained. Regardless of the merits of such innovations, she was not surprised at patient reactions knowing full well what makes the place tick.
“Patients just showed up anyway! It’s a second home for many and when they said,” I want to see my doctor” they meant it, and we couldn’t just shut down or control every aspect of how things functioned. People were scared. If you’re a patient here you want answers, and you want them from the people you know.” she spoke. “So, we did the best we could and kept thinking about how we could best prevent issues that would require an ER and provide the best outcomes.”
Jocelyn Guggenheim was both the English major writing and communicated protocols while very much the nurse thinking carefully about each patient, and all while having two young children at home.
“We didn’t know as much as we know, and it still changes. So, at the beginning we called every one of the highest risk patients every day. The nurses could hear when someone wasn’t breathing correctly and that some just weren’t ok. You feel the weight of that,” she said softly and purposefully. “It is like a family, and for some, we were it.”
Telehealth became a way of doing some healthcare and was a relief to those who had to work and avoid the ever-present parking issues, but social justice and equity is another guiding principle to the work. “Of course, for some telehealth is better and for some not. There are families without reliable internet who may need the care the most,” she said.
Seeing the work pace and quality of attention of this professional one surely has a sense of how others benefit from her impressive skill. But she is equally articulate and perceptive about her own changes as she is about systems and patients.
“I was so tired, but it was so gratifying, she said, recounting the navigation of testing and vaccines. “The Pfizer vials were an iconic moment,” she said of the unknown vaccine for a mysterious illness in a community expecting the best of care.
“I became more resilient. It showed me I could do really hard things and also that I had to take care of myself,” she said
Think about quitting? ‘No, I couldn’t leave my team” she said in a split second. Along with Nisha Thakkar, MD, and nursing team of Andrea Smith, and Elizabeth Martin and teams upon teams, the glue was the fact that “we were in the trenches together,” she said.
And so, with the support of her husband, Evan, and the amazingly resourceful team of those in every position at the South Boston Community Health Center, it became clearer than ever why this model of care helps neighbors regardless of status and health. It is the patients, creativity and team that compels Jocelyn Guggenheim to look at each patient carefully while preparing for ever more responsive ways of working at a place she knew she couldn’t leave the first time she entered.
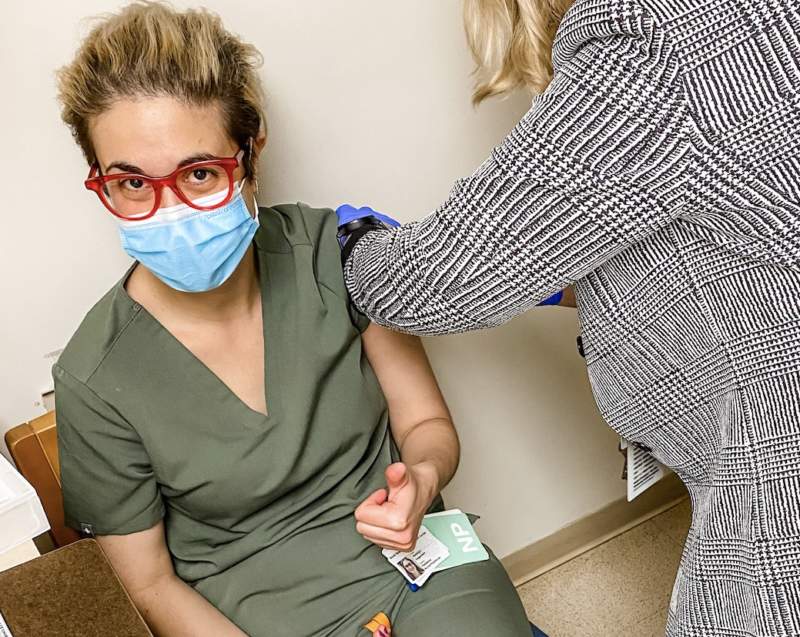
Jocelyn Guggenheim getting the vaccine in the midst of COVID Crisis.






